Why Senior Oral Health Matters
Keeping your mouth healthy after 65 isn’t just about a smile—it protects your body. Gum disease, affecting two‑thirds of seniors, can fuel inflammation that raises the risk of heart attacks, stroke, lung disease and dementia. About 20 % of adults over 65 experience dry mouth, and many also report tooth sensitivity from receding gums or grinding; both conditions make decay and discomfort more likely. A senior‑focused routine aims to control plaque, stay hydrated, and protect exposed teeth. Brush twice with a soft‑bristled brush, floss or use interdental cleaners each day, sip water frequently, chew sugar‑free gum, and see the dentist at least every six months for cleanings, exams and fluoride treatments.
Managing Xerostomia – Immediate Relief and Overnight Care
Quick‑Reference Tables for Xerostomia
Immediate Relief (Daytime)
| Action | How to Do It | Why It Helps |
|---|---|---|
| Sip water frequently | Keep a bottle handy and sip sip few510 anti every.30‑60 min | Directly moistens oral tissues |
| Chew sugar‑free gum / suck xylitol lozenges | 5‑10 min after meals or as needed | Stimulates salivary glands |
| Alcohol‑free fluoride mouthwash | Rinse for 30 sec, don’t swallow | Provides fluoride & moisture |
| OTC saliva substitutes (sprays, gels) | Apply per product directions (usually 2‑4 sprays) | Coats mucosa with lubricating agents |
| Avoid caffeine, alcohol, tobacco | Limit or eliminate intake | Reduces diuretic effect & dryness |
Nighttime Care
| Action | How to Do It | Why It Helps |
|---|---|---|
| Bedside humidifier | Run 1‑2 hrs before sleep at 30‑40 % RH | Keeps ambient air moist |
| Water spray bottle (glycerin or aloe) | Lightly mist mouth before lying down | Adds a protective film |
| Sugar‑free gum or xylitol lozenge before bed | Chew 5‑10 min or let lozenge dissolve | Promotes saliva flow overnight |
| Glycerin‑water spray or salt‑baking‑soda rinse | Spray or rinse 5‑10 min before sleep | Extra coating and pH balance |
| Prescription sialagogues (pilocarpine, cevimeline) | Take as dentist prescribes | Pharmacologic stimulation of saliva |
Dry‑Mouth Spray Options
| Product | Type | Duration of Moisture |
|---|---|---|
| Allday Dry Mouth Spray | OTC | ~2 hrs |
| Biotene Moisturizing Spray | OTC | ~2‑3 hrs |
| CVS Dry Mouth Spray | OTC | ~2 hrs |
| Aquoral Protective Oral Spray | Prescription (lipid‑based) | 4‑6 hrs |
Natural Remedies & Home Rinse
| Remedy | Ingredients | Application |
|---|---|---|
| Warm water + pinch of salt + baking soda | 1 tsp salt, ½ tsp baking soda, 8 oz warm water | Rinse 30 sec, spit out |
| Herbal tea (ginger) | Fresh ginger slices | tea |
| Humidifier + glycerin drops | 2‑3 drops glycerin in water spray | Light mist mouth |
Fastest Cure Summary
- Continuous moisture: sip water, use plain‑water spray, chew sugar‑free gum.
- Add humidifier at night.
- Eliminate diuretics (caffeine, alcohol).
- If inadequate, consult dentist for pilocarpine/cevimeline.
 How do I get rid of dry mouth ASAP?
How do I get rid of dry mouth ASAP?
Sip water frequently, keep a humidifier running at night, and lightly mist your mouth with a water spray. Chew sugar‑free gum or suck on xylitol lozenges to stimulate saliva. Use alcohol‑free fluoride mouthwash and over‑the‑counter saliva substitutes such as Biotene sprays. Avoid caffeine, alcohol, and tobacco, which worsen dryness.
Effective remedies for dry mouth at night
Place a bedside humidifier or personal misting bottle to keep oral tissues moist while you sleep. Before bed, sip water or a sugar‑free electrolyte drink and keep a glass nearby. Chew sugar‑free gum or use a saliva‑stimulating lozenge with xylitol or aloe. Apply a glycerin‑water spray or a homemade salt‑baking‑soda rinse for extra coating. For persistent symptoms, a dentist may prescribe pilocarpine or cevimeline.
Dry mouth spray options
Try over‑the‑counter sprays such as Allday Dry Mouth Spray, Biotene Moisturizing Spray, or CVS Dry Mouth Spray. Prescription‑strength options like Aquoral Protective Oral Spray provide a lipid‑based coating lasting 4‑6 hours. Discuss any chronic xerostomia with your dentist for a personalized plan.
Saliva substitutes for dry mouth
OTC substitutes (sprays, gels, rinses) contain xylitol, carboxymethylcellulose, or hydroxyethyl cellulose to lubricate the mouth. Examples include Biotene Rinse, Mouth Kote, Oasis Spray, and Biotene Gel. Use as needed, waiting 15 minutes before eating. Severe cases may require prescription sialagogues (pilocarpine, cevimeline).
Natural remedies for dry mouth at night
Use a bedside humidifier and a water spray bottle with a few drops of glycerin or aloe. Chew sugar‑free xylitol gum, sip water or herbal tea (e.g., ginger), and avoid evening caffeine/alcohol. A simple rinse of warm water, a pinch of salt, and baking soda can coat the oral mucosa and retain moisture throughout the night.
Fastest way to cure dry mouth
Keep the mouth continuously moisturized: sip water, use a plain‑water spray, chew sugar‑free gum, and apply an OTC saliva substitute. Add a humidifier and eliminate diuretics such as caffeine and alcohol. If relief is insufficient, consult your dentist about prescription options like pilocarpine for rapid saliva stimulation.
Regular Dental Visits and Access to Care
Dental‑Visit Frequency & Access Resources
| Category | Recommendation | Rationale |
|---|---|---|
| Standard seniors (≥65 y) | Twice a year (every 6 months) | Early detection of decay, gum disease, oral cancer |
| High‑risk seniors (diabetes, heart disease, xerostomia) | Every 3‑4 months or as dentist advises | Faster progression of periodontal disease & caries |
| New denture wearers | Every 6 months + after adjustments | Ensure proper fit & prevent sores |
Free / Low‑Cost Care Options
| Resource | Service Type | How to Access |
|---|---|---|
| Federally Qualified Health Centers (FQHC) | Sliding‑scale exams & cleanings | Locate via HRSA website |
| State Dental Assistance Programs | Medicaid‑eligible or low‑income adults | Apply through state health department |
| Eldercare Locator (US) | Referral to local free clinics | Call 1‑800‑677‑2699 or online portal |
| 2‑1‑1 Referral Lines | Community health resources | Dial 2‑1‑1 in your area |
| Oral Health America (non‑profit) | Care‑finder tool | Visit oralhealthamerica.org |
| Medicare Advantage Plans | Expanded dental benefits (often 70 % full coverage |
Key Take‑aways
- Routine visits are essential for preventing complications.
- Additional exams are warranted when systemic health issues affect oral health.
- Community resources can offset out‑of‑pocket costs.
 Seniors should see a dentist at least twice a year—generally every six months—to keep gum disease, dry mouth, and denture problems in check. If an 80‑year‑old has chronic illnesses such as diabetes, heart disease, or takes medications that reduce saliva, more frequent exams may be needed to catch early decay or oral cancer.
Seniors should see a dentist at least twice a year—generally every six months—to keep gum disease, dry mouth, and denture problems in check. If an 80‑year‑old has chronic illnesses such as diabetes, heart disease, or takes medications that reduce saliva, more frequent exams may be needed to catch early decay or oral cancer.
How often should an 80‑year‑old go to the dentist? An 80‑year‑old should schedule a dental check‑up at least twice a year, typically every six months. At this age, the risk of dry mouth, gum recession, and wear on existing restorations or dentures increases, so regular cleanings and exams help catch problems early. If the senior has chronic conditions such as diabetes, heart disease, or takes medications that affect oral health, more frequent visits may be advisable. The dentist will also monitor for oral cancer, assess the fit of any dentures, and provide personalized hygiene guidance. Maintaining this routine helps preserve comfort, function, and overall health well into the later years.
Free dental care for senior citizens While Medicare’s original plan rarely covers routine cleanings or fillings, seniors can still access free or low‑cost dental care through community resources. Federally qualified health centers, state‑run dental assistance programs, the Eldercare Locator, and 2‑1‑1 referral lines often offer sliding‑scale services. Non‑profits such as Oral Health America provide care‑finder tools, and many Medicare Advantage plans include expanded dental benefits, giving seniors additional coverage options. Exploring these resources helps older adults keep their smiles healthy without overwhelming out‑of‑pocket costs.
Understanding and Treating Tooth Sensitivity
Tooth Sensitivity vs. Toothache & Treatment Options
Quick‑
Decision Tree
| Symptom | Trigger | Duration | Likely Cause |
|---|---|---|---|
| Sharp, brief sting | Hot, cold, sweet, acidic foods/drinks | Disappears when stimulus removed | Tooth Sensitivity (exposed dentin) |
| Lingering throbbing pain | May occur without stimulus | Persists for minutes‑hours | Toothache (cavity, cracked tooth, infection) |
Desensitizing Agents (OTC)
| Brand | Active Ingredient | Mechanism |
|---|---|---|
| Sensodyne | Potassium nitrate | Blocks nerve transmission |
| Crest Sensitive | Stannous fluoride | Forms protective mineral layer |
| Biotene (for dry mouth) | Xylitol & fluoride | Lubricates + remineralizes |
Professional Options
| Procedure | When Used | Benefits |
|---|---|---|
| Fluoride varnish (0.4 % stannous) | Mild–moderate sensitivity, especially with xerostomia | Strong enamel reinforcement |
| Fluoride gel/varnish (1.1 % sodium) | Severe sensitivity, high caries risk | Long‑lasting protection |
| Bonding agents / sealants | Exposed root surfaces | Physical barrier |
| Crowns | Deep decay or structural loss | Full coverage & strength |
| Gum grafts | Recessed gums exposing roots | Restores tissue & reduces sensitivity |
Brand Comparison (Sensodyne vs. Crest)
| Feature | Sensodyne (Potassium nitrate) | Crest Sensitive (Stannous fluoride) |
|---|---|---|
| Onset of relief | 1‑2 weeks (fast for mild) | 2‑3 weeks (slower) |
| Enamel strengthening | Minimal | Moderate (stannous deposits) |
| Additional benefits | Extra Whitening line (higher price) | Whitening option available |
| Best for | Mild sensitivity, quick relief | Sensitivity + preventive enamel care |
Managing Dry Mouth in Sensitive Teeth
- Sip water frequently.
- Chew sugar‑free xylitol gum.
- Use alcohol‑free fluoride mouthwash.
- Apply OTC saliva substitutes before brushing.
Bottom Line: Identify the pain type, start with an OTC desensitizing toothpaste, consider professional fluoride or restorative care for persistent cases, and control xerostomia to protect exposed dentin.
 Seniors often wonder whether a sharp, brief pain is a toothache or simple tooth sensitivity. Sensitivity is a quick, sharp sting that appears only when hot, cold, sweet, or acidic stimuli touch an exposed dentin surface and disappears once the trigger is removed. A toothache, by contrast, is a lingering throbbing or sharp discomfort that can occur without stimulus and often signals deeper problems such as cavities, cracked teeth, infection, or gum disease.
Seniors often wonder whether a sharp, brief pain is a toothache or simple tooth sensitivity. Sensitivity is a quick, sharp sting that appears only when hot, cold, sweet, or acidic stimuli touch an exposed dentin surface and disappears once the trigger is removed. A toothache, by contrast, is a lingering throbbing or sharp discomfort that can occur without stimulus and often signals deeper problems such as cavities, cracked teeth, infection, or gum disease.
Desensitizing agents—like potassium nitrate in Sensodyne and stannous fluoride in Crest Sensitive—work by blocking nerve signals or reinforcing enamel. Over‑the‑counter desensitizing toothpaste can provide relief for mild cases, while prescription‑strength fluoride gels or varnishes (0.4% stannous fluoride or 1.1% sodium fluoride) offer stronger protection for seniors with dry mouth or root exposure.
Professional options include fluoride varnish, bonding agents, sealants, or crowns to cover exposed roots. For severe gum recession, gum grafts may be recommended.
Brand comparison: Sensodyne’s potassium‑nitrate formula often gives faster relief for mild sensitivity, whereas Crest Sensitive’s stannous‑fluoride formulation adds enamel‑strengthening benefits and may better prevent future decay. Crest also offers whitening, while Sensodyne’s Extra Whitening line is slightly pricier.
Dry mouth (xerostomia) is a red flag for medication side effects, diabetes, autoimmune disease, or radiation damage, and it heightens decay risk. Seniors should sip water, chew sugar‑free gum, and use alcohol‑free fluoride mouthwash to stimulate saliva and protect teeth.
Bottom line: Identify whether pain is sensitivity or a toothache, use a desensitizing toothpaste, consider professional fluoride or restorative care, and manage dry mouth to keep teeth strong and comfortable.
Optimizing Daily Oral Hygiene for Seniors
Daily Oral‑Hygiene Checklist for Seniors
| Task | Frequency | Recommended Tool / Product | Tips |
|---|---|---|---|
| Brushing | Twice daily (morning & night) | Soft‑/extra‑soft‑bristled electric toothbrush with timer | 45° angle, gentle circular motions, 2 min per session |
| Flossing / Interdental cleaning | Daily | Interdental brushes, floss picks, or water flosser | Choose size that fits comfortably; water flosser helpful for limited dexterity |
| Mouthwash (alcohol‑free fluoride) | After brushing or as needed | Alcohol‑free fluoride rinse (e.g., Biotene) | Swish 30 sec, do not swallow |
| Hydration | Throughout day | Plain water, sugar‑free electrolyte drinks | Sip regularly, especially after meals |
| Saliva stimulation | As needed | Sugar‑free xylitol gum or lozenges | Chew 5‑10 min after meals |
| Denture care (if applicable) | Daily | Soft denture brush + soaking solution | Rinse after meals, soak overnight |
Systemic Health Connection
| Condition | Oral‑Hygiene Impact |
|---|---|
| Heart disease & stroke | Bacterial translocation from gingivitis can exacerbate atherosclerosis |
| Diabetes | Poor oral hygiene raises blood‑glucose levels and infection risk |
| Cognitive decline | Inflammation from oral infections may contribute to neurodegeneration |
| Nutrition | Tooth pain or dry mouth can limit food choices, leading to malnutrition |
Quick‑Boosters for Gum Health
- Use a fluoride mouthwash daily.
- Rinse with plain water before brushing to dislodge debris.
- Chew sugar‑free gum after meals.
- Limit sugary/acidic beverages and quit tobacco.
Reminder
- Schedule professional cleaning & exam every 6 months.
- Communicate any new pain, dryness, or changes to your dentist promptly.
 Maintaining good oral hygiene is essential for seniors because gum disease, tooth decay, and dry mouth become more common with age. Brushing twice a day with a soft‑ or extra‑soft‑bristled toothbrush—ideally an electric model with a timer or a grip‑aid handle—helps remove plaque without irritating receded gums. Hold the brush at a 45‑degree angle to the gum line and use gentle, circular motions for at least two minutes. For those with limited dexterity, flossing can be replaced by interdental brushes, floss picks, or a water flosser, all of which reach between teeth where a traditional string floss may be difficult.
Maintaining good oral hygiene is essential for seniors because gum disease, tooth decay, and dry mouth become more common with age. Brushing twice a day with a soft‑ or extra‑soft‑bristled toothbrush—ideally an electric model with a timer or a grip‑aid handle—helps remove plaque without irritating receded gums. Hold the brush at a 45‑degree angle to the gum line and use gentle, circular motions for at least two minutes. For those with limited dexterity, flossing can be replaced by interdental brushes, floss picks, or a water flosser, all of which reach between teeth where a traditional string floss may be difficult.
Quick gum‑health boosters include daily use of an alcohol‑free fluoride mouthwash, rinsing with plain water before brushing to dislodge food particles, and chewing sugar‑free gum to stimulate saliva flow. Staying well‑hydrated, limiting sugary or acidic drinks, and quitting tobacco further protect the gums.
Why is this especially important for older adults? Poor oral hygiene can let harmful bacteria enter the bloodstream, increasing the risk of heart disease, stroke, diabetes complications, and even cognitive decline. Keeping the mouth clean also prevents pain, tooth loss, and infections such as thrush, allowing seniors to maintain a nutritious diet and overall health. Regular dental check‑ups every six months provide professional cleanings, fluoride treatments, and early detection of problems, reinforcing the link between a healthy smile and a healthy body.
Caregiver Strategies and Dental Technologies for Seniors
Caregiver‑Focused Oral‑Care Guide & Dry‑Mouth Products
Oral Care Routine for Seniors with Dementia
| Step | Action | Assistive Technique |
|---|---|---|
| 1. Brushing | Use a soft‑bristled or children’s toothbrush | Watch‑me: demonstrate brushing motion before patient attempts |
| 2. Toothpaste | Apply a pea‑size amount of non‑irritating, fluoride toothpaste | Use a small squeeze‑tube for easy dispensing |
| 3. Interdental cleaning | Choose floss picks, tiny interdental brushes, or a water flosser | Water flosser reduces manual dexterity demand |
| 4. Denture care | Remove, rinse, brush, and soak overnight in cleanser | Label denture with color‑coded holder to avoid mix‑up |
| 5. Moisturizing | Apply dry‑mouth spray or gel after brushing | Keep spray within easy reach; use a pump for quick mist |
| 6. Reinforcement | Provide positive verbal cues and short reminders | Use a visual schedule with pictures of each step |
Dry‑Mouth Treatment Products (OTC & Prescription)
| Product | Form | Key Ingredients | Approx. Duration of Moisture |
|---|---|---|---|
| Biotène Oralbalance Gel | Gel | Xylitol, carboxymethylcellulose | 2‑3 hrs |
| Biotène Moisturizing Spray | Spray | Glycerin, aloe vera | 2‑3 hrs |
| Allday Dry Mouth Spray | Spray | Glycerin, propylene glycol | 2‑3 hrs |
| ACT Dry Mouth Lozenges | Lozenge | Xylitol, sorbitol | Stimulates saliva for 30‑60 min |
| Biotène Fluoride Toothpaste | Toothpaste | Sodium fluoride, xylitol | Continuous protection |
| Oracoat XyliMelts (Adherent discs) | Disc (night use) | Xylitol, glycerin | Up to 8 hrs |
| Aquoral Protective Oral Spray (Prescription) | Spray | Lipid‑based coating | 4‑6 hrs |
Tips for Caregivers
- Timing: Apply moisturizers after brushing and before bedtime.
- Monitoring: Check for oral sores, redness, or signs of infection daily.
- Communication: Keep the dentist informed about medication changes that may affect saliva.
- Education: Show patients the difference between a spray (quick mist) and a gel (longer coating) to match preferences.
Technology Aids
- Electric toothbrushes with large grips and audible timers.
- Water flossers with adjustable pressure settings.
- Smartphone reminder apps for brushing and medication schedules.
- Tele‑dentistry for quick consults when in‑person visits are challenging.
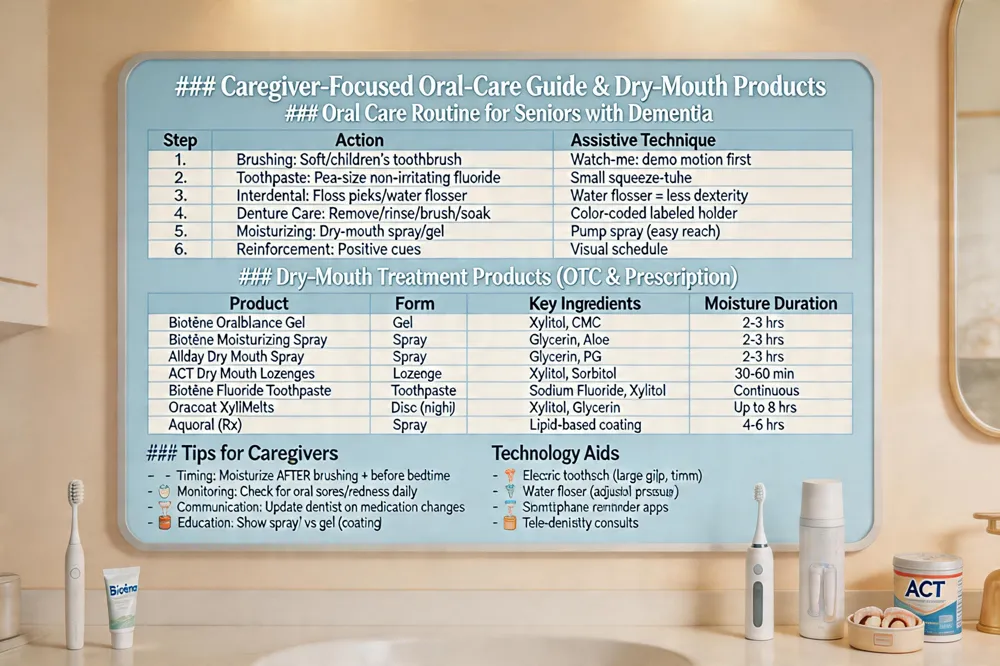 Oral care for elderly with dementia
Good oral hygiene is essential for seniors with dementia because it prevents infections, eases eating, and can reduce costly dental procedures. Caregivers should set a simple twice‑daily brushing routine using a soft‑bristled or children’s toothbrush. Offer short, step‑by‑step instructions and use the “watch‑me” technique so the patient sees the motion before trying it. For interdental cleaning, choose floss, tiny interdental brushes, or a water flosser that requires less manual dexterity. Denture wearers need daily rinsing, brushing, and overnight soaking in a cleanser. Moisturizing products such as dry‑mouth sprays help counteract medication‑induced dryness, and a gentle, non‑irritating toothpaste reduces resistance. Communicate openly with the dentist about the patient’s dementia stage so treatment plans can be adjusted for comfort and safety.
Oral care for elderly with dementia
Good oral hygiene is essential for seniors with dementia because it prevents infections, eases eating, and can reduce costly dental procedures. Caregivers should set a simple twice‑daily brushing routine using a soft‑bristled or children’s toothbrush. Offer short, step‑by‑step instructions and use the “watch‑me” technique so the patient sees the motion before trying it. For interdental cleaning, choose floss, tiny interdental brushes, or a water flosser that requires less manual dexterity. Denture wearers need daily rinsing, brushing, and overnight soaking in a cleanser. Moisturizing products such as dry‑mouth sprays help counteract medication‑induced dryness, and a gentle, non‑irritating toothpaste reduces resistance. Communicate openly with the dentist about the patient’s dementia stage so treatment plans can be adjusted for comfort and safety.
Dry mouth treatment products Dry mouth (xerostomia) can be managed with over‑the‑counter options that lubricate oral tissues and protect teeth. Moisturizing gels (e.g., Biotène Oralbalance), sprays (Biotène Moisturizing Spray), and alcohol‑free rinses provide long‑lasting relief and match the pH of natural saliva. Sugar‑free gum and xylitol‑sweetened lozenges (ACT Dry Mouth Lozenges) stimulate saliva, while saliva‑substituting sprays (Allday Dry Mouth Spray) replace it. Fluoride toothpaste and rinses, such as Biotène fluoride toothpaste, help prevent decay when mouth is dry. For nighttime comfort, adherent discs (Oracoat XyliMelts) or a thick gel applied before bed can offer up to eight hours of moisture.
A Healthy Future Starts with Informed Care
Staying well‑hydrated, practicing gentle brushing with a soft‑bristled or electric toothbrush, and flossing daily keep a mouth clean and protect vulnerable teeth. Regular use of fluoride toothpaste, alcohol‑free mouthwash, and saliva‑stimulating gum further reduces decay and sensitivity, especially when dry mouth is present. Visiting a dentist twice a year for cleanings, X‑rays, and personalized fluoride treatments catches problems early and supports overall health. Local senior centers, community health clinics, and pharmacy programs often offer oral‑health workshops and discounted supplies that can help you maintain these habits. Call Loud Family Dental today to schedule a personalized visit and receive a tailored care plan for your bright, healthy smile, and confidence today.
